
DIseases
Vaginismus: Causes of Vaginal Narrowing
Many women have heard of erectile dysfunction, which occurs in men when they cannot have an erection. Generally, the causes of impotence are usually psychological

Many women have heard of erectile dysfunction, which occurs in men when they cannot have an erection. Generally, the causes of impotence are usually psychological
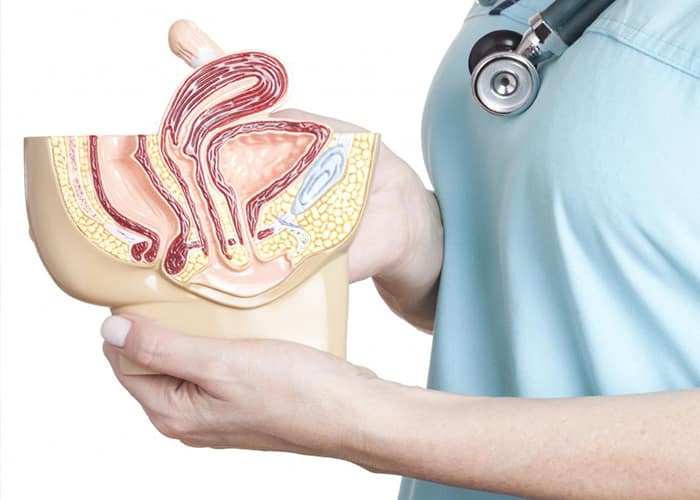
We know that typically, the female anatomy can vary a bit from woman to woman: larger or smaller breasts, a higher or lower cervix, a